Menopause can be a challenging time for many women, as it often brings about hormonal changes that can impact various aspects of their health. One area that can be particularly affected is cholesterol levels. High cholesterol is a concern for many individuals, as it is a major risk factor for heart disease. During menopause, hormonal fluctuations can lead to changes in cholesterol levels, making it essential to manage them effectively. In this article, we will explore some practical tips and strategies to help you keep your cholesterol levels in check during menopause and navigate this transitional phase with confidence and good health.

Understanding Cholesterol and Menopause
During menopause, a woman’s body goes through various hormonal changes that can have an impact on cholesterol levels. Cholesterol is a waxy substance that is naturally produced in the body and plays a vital role in the formation of cell membranes, hormone production, and the synthesis of vitamin D. However, when cholesterol levels become imbalanced, it can increase the risk of developing heart disease and other related health issues.
Role of Cholesterol in the Body
Cholesterol is a crucial component of our body’s functioning. It serves as a building block for cell membranes, helping to maintain their integrity and fluidity. Cholesterol also plays a key role in the production of hormones such as estrogen, progesterone, and testosterone. Additionally, it aids in the synthesis of vitamin D, which is essential for bone health and immune function.

Impact of Menopause on Cholesterol Levels
Menopause is a natural phase of a woman’s life that typically occurs between the ages of 45 and 55. During this time, the ovaries gradually cease to produce estrogen and progesterone, leading to a range of physical and emotional changes. These hormonal changes can also affect cholesterol levels, often resulting in an unfavorable lipid profile.
Understanding Hormonal Changes during Menopause
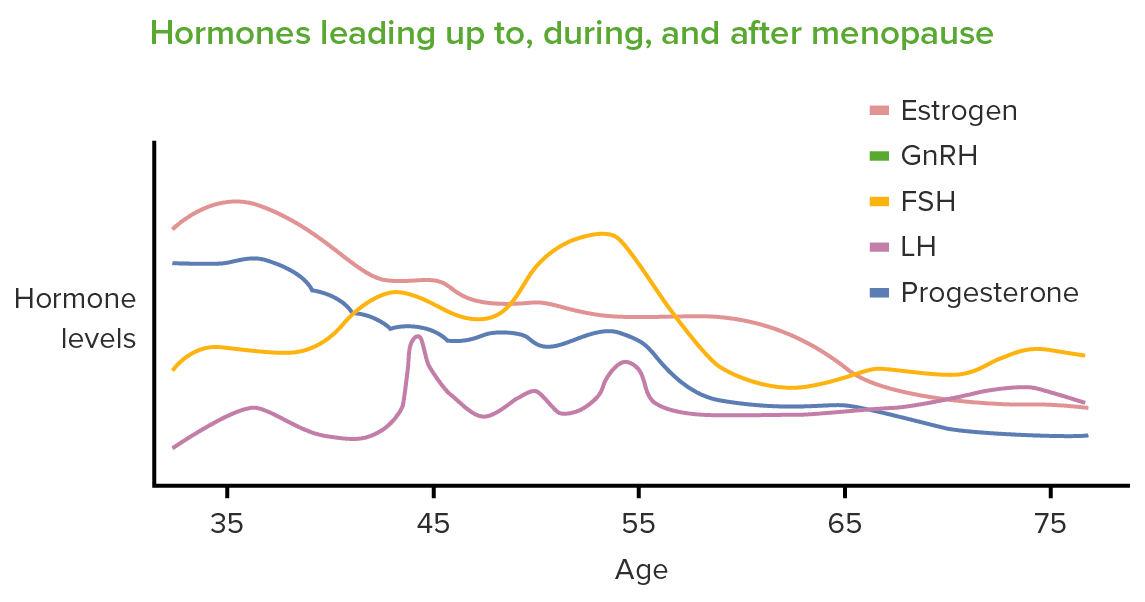
The hormonal changes that occur during menopause significantly impact cholesterol levels. Estrogen, a hormone primarily produced by the ovaries, plays a crucial role in maintaining a healthy lipid profile. However, as estrogen levels decline during menopause, the balance between good (HDL) and bad (LDL) cholesterol can be disrupted. This hormonal imbalance can lead to an increase in total cholesterol, LDL cholesterol, and triglyceride levels, while reducing the levels of HDL cholesterol.
Effect of Hormonal Changes on Cholesterol
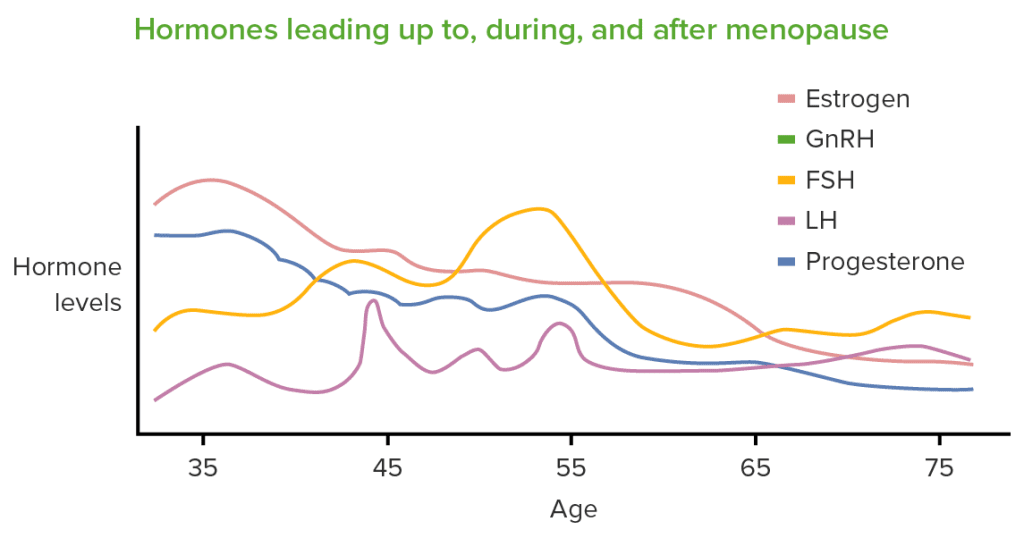
Decreased Estrogen Levels
Decreased levels of estrogen during menopause have a significant impact on cholesterol metabolism. Estrogen promotes the production of HDL cholesterol, which helps remove LDL cholesterol from the bloodstream. When estrogen levels decline, this balance is disrupted, leading to higher levels of LDL cholesterol and a decrease in HDL cholesterol.
Increased LDL Cholesterol
LDL cholesterol, commonly known as “bad cholesterol,” is responsible for the accumulation of plaque in the arteries, leading to atherosclerosis and an increased risk of heart disease. The hormonal changes during menopause can elevate LDL cholesterol levels, contributing to a higher risk of cardiovascular complications.
Decreased HDL Cholesterol
HDL cholesterol, often referred to as “good cholesterol,” plays a crucial role in cardiovascular health by helping to remove excess cholesterol from the bloodstream. However, during menopause, decreased estrogen levels can lead to a reduction in HDL cholesterol, further exacerbating the imbalance between good and bad cholesterol.
Increased Triglycerides
Triglycerides are a type of fat found in the bloodstream that can contribute to the narrowing of arteries and increase the risk of cardiovascular disease. Hormonal changes during menopause can lead to elevated triglyceride levels, which, when combined with high LDL cholesterol and low HDL cholesterol, can further increase the risk of heart disease.
Dietary Changes to Manage Cholesterol
Adopting a heart-healthy diet can play a significant role in managing cholesterol levels during menopause. Here are some dietary changes you can make:
Choose Heart-Healthy Fats
Opt for sources of healthy fats such as avocados, nuts, seeds, and olive oil. These fats can help raise HDL cholesterol levels and reduce LDL cholesterol levels.
Increase Dietary Fiber
Include more fiber-rich foods in your diet, such as whole grains, fruits, vegetables, and legumes. Soluble fiber can help lower LDL cholesterol levels by binding to cholesterol in the digestive system and eliminating it from the body.
Consume Omega-3 Fatty Acids
Omega-3 fatty acids, found in fatty fish like salmon and trout, can help lower triglyceride levels and reduce inflammation in the body. Consider including fish in your diet or talking to your healthcare provider about omega-3 supplements.
Avoid Trans Fats and Saturated Fats
Limit your intake of trans fats and saturated fats, often found in processed and fried foods, baked goods, and fatty meats. These fats contribute to higher LDL cholesterol levels and increase the risk of heart disease.
Limit Dietary Cholesterol Intake
While dietary cholesterol has less impact on blood cholesterol levels than previously thought, it’s still beneficial to monitor your intake. Limit foods high in cholesterol, such as organ meats, shellfish, and high-fat dairy products.
Regular Exercise and Physical Activity
Engaging in regular exercise and physical activity is another essential aspect of managing cholesterol levels during menopause. Exercise offers numerous benefits for heart health and cholesterol management.
Aerobic Exercise
Engage in aerobic activities such as brisk walking, jogging, cycling, swimming, or dancing. Aim for at least 150 minutes of moderate-intensity aerobic exercise or 75 minutes of vigorous-intensity aerobic exercise per week.
Strength Training
Incorporate strength training exercises into your routine to build and maintain muscle mass. Strength training can help improve insulin sensitivity and raise HDL cholesterol levels.
Benefits of Exercise for Cholesterol Levels
Regular exercise can increase HDL cholesterol levels, improve overall lipid profiles, and lower levels of triglycerides and LDL cholesterol. These benefits contribute to a lower risk of heart disease.
Recommended Exercise Guidelines
Consult with your healthcare provider to determine the most appropriate exercise routine for your specific needs and abilities. They can provide personalized recommendations based on your health status and any underlying conditions.
Lifestyle Modifications
Making certain lifestyle modifications can further support cholesterol management during menopause. Consider the following changes:
Maintain a Healthy Weight
Achieving and maintaining a healthy weight can help improve cholesterol levels and overall cardiovascular health. Aim for a balanced diet, regular exercise, and portion control to manage your weight effectively.
Quit Smoking
Smoking is a significant risk factor for heart disease and can worsen the impact of hormonal changes on cholesterol levels. Quitting smoking can improve both your cholesterol profile and your overall health.
Limit Alcohol Consumption
Excessive alcohol consumption can raise triglyceride levels and contribute to unfavorable changes in cholesterol levels. Limit your alcohol intake to moderate levels, as recommended by healthcare professionals.
Manage Stress Levels
Chronic stress can increase the risk of heart disease and impact cholesterol levels. Find healthy ways to manage stress, such as engaging in relaxation techniques or seeking support from friends, family, or healthcare professionals.
Supplements for Cholesterol Management
In addition to lifestyle modifications, certain supplements may be considered to support cholesterol management during menopause. However, it is essential to consult with your healthcare provider before beginning any new supplements. Some common supplements include:
Plant Sterols and Stanols
Plant sterols and stanols are naturally occurring compounds found in plant-based foods. They can help lower LDL cholesterol levels by blocking cholesterol absorption in the digestive system. These supplements are available in various forms such as fortified foods or dietary supplements.
Omega-3 Fatty Acid Supplements
Supplements containing omega-3 fatty acids, such as fish oil capsules, may help lower triglyceride levels and have a positive impact on overall heart health. Discuss the appropriate dosage and form of omega-3 supplements with your healthcare provider.
Red Yeast Rice
Red yeast rice is a traditional Chinese medicine made from fermented rice. It contains a compound called monacolin K, which is similar to a commonly used cholesterol-lowering medication called lovastatin. However, it’s important to note that red yeast rice supplements can vary in their composition and potency, so consulting with your healthcare provider is crucial.
Garlic Supplements
Garlic has long been associated with various health benefits, including potential cholesterol-lowering effects. Garlic supplements may modestly reduce total cholesterol and LDL cholesterol levels. However, the evidence is still evolving, and it’s best to consult with your healthcare provider regarding the use of garlic supplements.
Coenzyme Q10
Coenzyme Q10, also known as CoQ10, is a natural antioxidant produced by the body. Some studies suggest that CoQ10 supplements may help reduce oxidative stress, improve lipid metabolism, and potentially benefit cholesterol management. However, further research is needed to establish its effectiveness.
Hormone Replacement Therapy (HRT)
Hormone replacement therapy (HRT) is a treatment option that involves taking estrogen or a combination of estrogen and progesterone to alleviate menopausal symptoms. It may also be considered for cholesterol management in certain cases. However, HRT comes with both benefits and risks, and it’s essential to discuss the potential impact on cholesterol levels with your healthcare provider.
Benefits and Risks of HRT
HRT can help relieve menopausal symptoms such as hot flashes, night sweats, and vaginal dryness. However, it also carries potential risks, including an increased risk of breast cancer, blood clots, stroke, and cardiovascular disease. It is crucial to carefully weigh the benefits and risks with your healthcare provider before considering HRT for cholesterol management.
Impact of HRT on Cholesterol Levels
HRT involving estrogen can have both positive and negative effects on cholesterol levels. While estrogen can raise HDL cholesterol levels, it can also increase triglyceride levels. Additionally, the use of combination hormone therapy (estrogen and progesterone) may result in a decrease in HDL cholesterol and an increase in LDL cholesterol.
Considerations for using HRT for Cholesterol Management
HRT should not be started solely for cholesterol management. It is typically reserved for managing menopausal symptoms in women who are also at low risk for cardiovascular disease. The decision to use HRT should be made in consultation with your healthcare provider, considering your individual health history, symptoms, and cholesterol profile.
Regular Cholesterol Monitoring
Regular monitoring of your cholesterol levels is essential to ensure effective management during menopause. Understanding your cholesterol profile and assessing any changes is crucial for making informed decisions about treatment approaches. Here are some key points to consider:
Understanding Cholesterol Profile
A comprehensive cholesterol profile includes measurements of total cholesterol, LDL cholesterol, HDL cholesterol, and triglyceride levels. These values provide healthcare providers with valuable information about your lipid profile and overall cardiovascular health.
Frequency of Cholesterol Testing
The frequency of cholesterol testing can vary depending on your individual risk factors and health history. In general, individuals without any significant cardiovascular risk factors should undergo cholesterol testing every five years. However, if there are specific concerns or an increased risk, more frequent testing may be necessary.
Consultation with Healthcare Provider
Discuss your cholesterol levels and any concerns with your healthcare provider. They can help interpret your test results, tailor treatment plans to your specific needs, and provide guidance on managing cholesterol levels during menopause and hormonal changes.
Medications for Cholesterol Management
In some cases, lifestyle modifications and supplements may not be sufficient to manage cholesterol levels effectively. Your healthcare provider may recommend cholesterol-lowering medications, such as statins or other types of medication.
Statins and Other Cholesterol-Lowering Drugs
Statins are a commonly prescribed class of medications for managing high cholesterol levels. They work by inhibiting an enzyme involved in cholesterol production in the liver. Other medications, such as bile acid sequestrants, cholesterol absorption inhibitors, and PCSK9 inhibitors, may also be prescribed based on individual needs and considerations.
Benefit-Risk Analysis of Medications
Before starting any medication, your healthcare provider will conduct a comprehensive benefit-risk analysis. This analysis takes into account your cholesterol levels, overall health, potential side effects of medications, and individual risk factors for heart disease.
Role of Medications during Menopause and Hormonal Changes
Medications for cholesterol management can be particularly beneficial for women going through menopause, as hormonal changes can cause significant fluctuations in lipid profiles. Your healthcare provider will determine the most appropriate medication, if necessary, considering the potential impact on cholesterol levels and overall cardiovascular health.
Consultation with Healthcare Professionals
Regular check-ups with healthcare professionals are crucial for managing cholesterol levels during menopause. These professionals can guide you through the various aspects of cholesterol management and help you make informed decisions.
Importance of Regular Check-ups
Regular check-ups allow healthcare professionals to assess your overall health, evaluate cholesterol levels, and review any necessary treatment modifications. These appointments also provide an opportunity to address any concerns or questions you may have.
Collaborate with Healthcare Provider for Personalized Management
Work closely with your healthcare provider to develop a personalized management plan for your cholesterol levels during menopause. They will consider your medical history, cholesterol profile, menopausal symptoms, and individual risk factors to create a tailored approach.
Discussing the Role of Menopause and Hormonal Changes in Cholesterol
Openly discuss the impact of menopause and hormonal changes on your cholesterol levels with your healthcare provider. Understanding the relationship between these factors is important for effective management and addressing any concerns you may have.
By adopting a comprehensive approach that includes lifestyle modifications, supplements (if appropriate), regular exercise, cholesterol monitoring, and collaboration with healthcare professionals, you can effectively manage cholesterol levels during menopause and hormonal changes. Remember, personalized care and regular communication with your healthcare provider are vital for optimizing your cholesterol management and overall cardiovascular health.